Although technology has made great progress in linking mental disorders with abnormal brain activity, there is still work to be done for diseases such as PTSD.
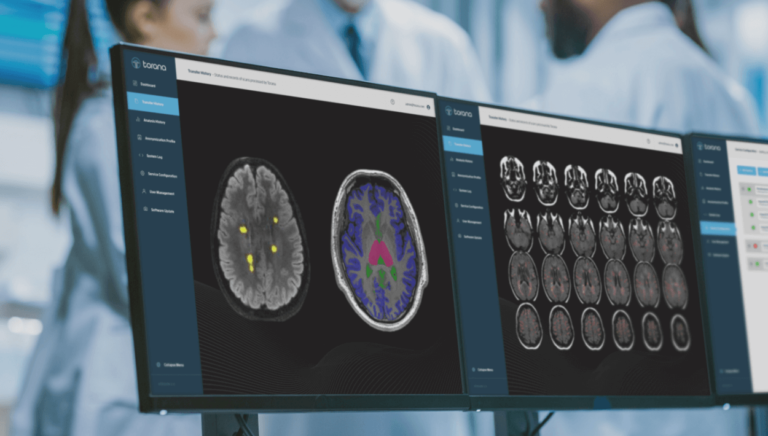
The neuroimaging technology is a promising tool for clinicians to link mental disorders with specific symptoms. A new study led by Yale shows that there are still kinks in the system before doctors can translate brain images to psychiatric conditions such as posttraumatic stress disorder (PTSD).
The findings were published in the American Journal of Psychiatry on January 11.
The National Institutes of Mental Health began a multibillion dollar research project several years ago to identify biomarkers of the brain that could point to biological roots of many mental illnesses. These diseases are currently identified through a clinical evaluation of symptoms, often overlapping, reported by patients.
Ilan Harpaz Rotem, Yale professor of psychiatry & psychology and senior author of this study, said: “The idea is that we forget classification of diseases by symptoms and look for underlying biological reasons.”
The Yale-led study attempted to replicate findings from an earlier neuroimaging study that linked clusters in brain activity with a range of outcomes for patients who arrived at U.S. ERs after traumatic events. Researchers measured brain activity of patients during simple tasks, including those that tested responses to rewards and threats. They detected a cluster that was highly reactive to both reward and threat signals.
Yale researchers were unable to reproduce these findings when they analyzed similar neuroimaging results collected from trauma survivors who had recently returned from Israel. They did identify the clusters of brain activities observed in the previous study but found no correlation with potential PTSD symptoms.
The study’s corresponding author, Ziv Ben Zion, is a postdoctoral fellow at Yale School of Medicine.
Ben-Zion explained that Yale researchers and the original Emory-Harvard investigators are merging datasets to “search for common underlying brain activity patterns associated with different responses” to trauma.
Harpaz-Rotem said that it took 100 years for mental illness to be classified in the way they are today. However, we have only been refining our psychiatric diagnosis using biomarkers over the past 10 years. “We have a lot of work to do.”
,